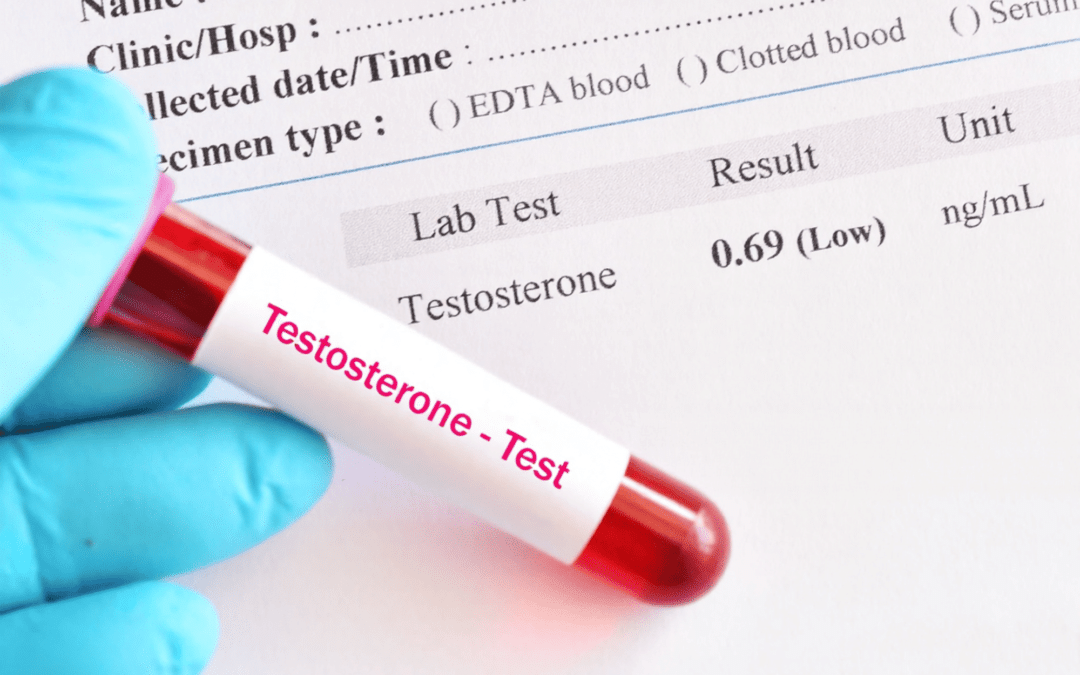
Most men who suspect low testosterone start with what they feel. Fatigue that lingers for months. A declining interest in sex. A general sense that something is off. These experiences are valid, and they deserve attention. But feeling the symptoms and confirming a low testosterone diagnosis are two very different steps. At Vivagen Health, we believe the path between suspicion and diagnosis should be built on clinical reasoning, not assumptions. Here is how that process actually works.
Why Many Men Jump to a Diagnosis Too Early
The gap between feeling off and having a confirmed diagnosis is wider than most men expect. Rushing through that gap often leads to misplaced confidence or unnecessary frustration.

Symptoms Can Feel Obvious Before the Cause Is Clear
Low energy, reduced libido, and increased body fat are commonly associated with low testosterone. When several of these symptoms appear together, it is natural to connect the dots. But the human body does not operate in straight lines. A cluster of symptoms that looks like low testosterone may stem from sleep disorders, thyroid imbalances, chronic stress, or even medication side effects. Jumping to a conclusion before testing can send someone down the wrong treatment path entirely.
>>> Read more: https://my.clevelandclinic.org/health/diseases/15216-low-libido-low-sex-drive
Online Content Encourages Self-Labeling
A quick search for “low testosterone symptoms” returns pages of content designed to confirm suspicion rather than challenge it. Symptom quizzes, listicles, and marketing funnels often lead readers toward a single conclusion before any lab work has been done. This kind of content can be useful for raising awareness, but it often skips the clinical thinking that distinguishes suspicion from diagnosis.
Confusion Delays Useful Answers
When men self-diagnose and then encounter conflicting information, many stall. They are not sure whether to see a urologist, an endocrinologist, or a primary care provider. Others order direct-to-consumer lab panels without understanding what the numbers mean. In both cases, confusion delays the evaluation that would actually give them clarity.

What Symptoms Can Tell You—and What They Cannot
Low testosterone symptoms are real and worth paying attention to. But their presence alone does not tell you the full story about what is happening inside your body.
Changes May Raise Suspicion
Symptoms serve a real purpose. They signal that something has shifted. The following are commonly reported by men who are later found to have low testosterone:
- Persistent fatigue unrelated to sleep habits
- Decreased sex drive or difficulty maintaining erections
- Loss of muscle mass despite consistent exercise
- Increased irritability or low mood
- Difficulty concentrating or recalling information
These patterns are worth noting and worth discussing with a qualified provider.
>>> Read more: https://www.urologyhealth.org/urology-a-z/l/low-testosterone
Several Issues Can Overlap
The challenge is that many of these same symptoms appear in other conditions. Consider how much overlap exists:
| Symptom | Low Testosterone | Thyroid Disorder | Depression | Sleep Apnea |
| Fatigue | Yes | Yes | Yes | Yes |
| Low libido | Yes | Sometimes | Yes | Yes |
| Weight gain | Yes | Yes | Sometimes | Yes |
| Brain fog | Yes | Yes | Yes | Yes |
| Mood changes | Yes | Yes | Yes | Sometimes |
This overlap is exactly why a testosterone evaluation must go beyond a symptom checklist.
Symptoms Start the Conversation, Not Finish It
Recognizing symptoms is the first step. But symptoms alone cannot confirm how low testosterone is diagnosed in a clinical setting. They open the door to investigation. What follows is where real answers begin.
>>> Read more: https://vivagenhealth.com/early-signs-of-low-testosterone/
What a Real Testosterone Evaluation Should Include
A proper testosterone evaluation is more than a blood draw. It involves structured clinical thinking that connects your symptoms, your bloodwork, and your overall health into a single picture.

Symptom History, Timing, Severity
A responsible evaluation starts with a thorough clinical interview. Your provider should ask when the symptoms began, how they have progressed, and how much they affect daily life. This context shapes everything that follows, from which labs to order to how results are interpreted.
Lab Work in Context
Blood testing is a central part of how low testosterone is diagnosed, but a single total testosterone number is rarely enough. A proper panel typically includes:
- Total testosterone to establish a baseline reading
- Free testosterone to assess what is biologically available
- SHBG (sex hormone-binding globulin) to understand how testosterone is being carried in the blood
- LH (luteinizing hormone) and FSH (follicle-stimulating hormone) to evaluate whether the brain is signaling the testes properly
- Estradiol to check for hormonal conversion issues
- CBC (complete blood count) and metabolic panel to screen for related health markers
Each of these values tells part of the story. Together, they form a clinical picture that a single number cannot provide.
Broader Look at Contributing Factors
Beyond bloodwork, a thorough evaluation considers lifestyle factors, existing medications, body composition, stress levels, and sleep quality. These inputs influence testosterone production and can shift how results are interpreted. A provider who skips this step risks treating a number instead of treating the patient.
>>> Read more: https://vivagenhealth.com/testosterone-blood-tests/
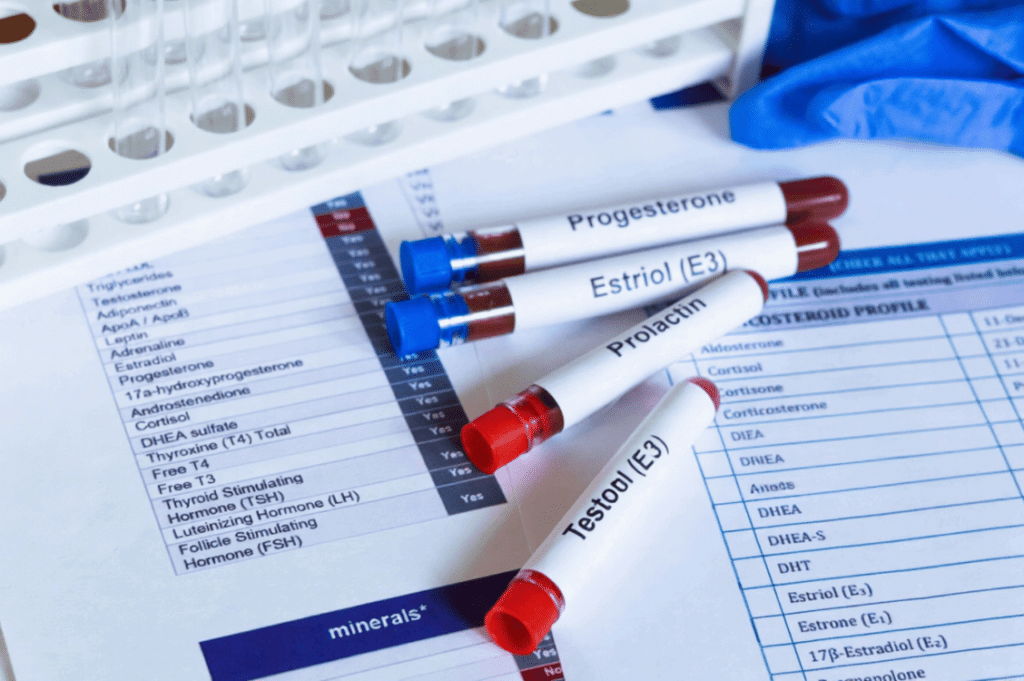
Why One Lab Result Rarely Answers Everything
Bloodwork is a powerful diagnostic tool, but a single snapshot rarely captures the full reality of your hormonal health. Understanding why requires looking at how testosterone behaves in the body.
Timing and Context Matter
Testosterone levels fluctuate throughout the day. They are typically highest in the early morning and can be influenced by recent illness, poor sleep, alcohol consumption, or acute stress. A single blood draw taken at 3 p.m. after a poor night of sleep may not reflect your actual hormonal baseline. That is why most guidelines recommend testing in the morning and repeating the draw on a separate day before making any clinical decisions.
Normal-Looking Results May Not Settle the Question
A testosterone reading within the standard reference range does not automatically rule out a problem. Reference ranges are broad, and a man whose levels have dropped significantly from his personal baseline may still fall within “normal” limits while experiencing meaningful symptoms. Context matters more than cutoff numbers.
Abnormal Results Still Need Interpretation
On the other side, a low number on a lab report does not automatically mean testosterone therapy is the right move. The result needs to be weighed against the full clinical picture. Is the low reading consistent across multiple tests? Are there reversible causes that should be addressed first? Is the pituitary gland functioning properly? These are the questions a qualified provider should be asking.
>>> Read more: https://www.health.harvard.edu/healthy-aging-and-longevity/testosterone–what-it-does-and-doesnt-do
What Usually Happens After the Evaluation
The outcome of a testosterone evaluation is not always a single, definitive answer. What happens next depends entirely on what the clinical findings reveal.
Sometimes Treatment Is Discussed
When lab results consistently show low testosterone, symptoms align with the clinical picture, and reversible causes have been considered, your provider may discuss testosterone therapy as a treatment option. This conversation should include expected outcomes, potential risks, monitoring protocols, and realistic timelines.
Sometimes More Clarification Is Needed
In many cases, the first round of testing raises new questions rather than closing the loop. A provider may recommend additional labs, imaging, or a referral to a specialist. This is a sign that your evaluation is being handled responsibly, not that something has gone wrong.
Sometimes Another Explanation Needs Ruling Out
Occasionally, the evaluation reveals that the symptoms are better explained by another condition entirely. Thyroid dysfunction, obstructive sleep apnea, clinical depression, or metabolic syndrome may be identified as the primary driver. Addressing the correct root cause leads to better results than treating the wrong diagnosis.
>>> Read more: https://my.clevelandclinic.org/health/diseases/8541-thyroid-disease
Schedule Your Testosterone Therapy Consultation
If your symptoms have been lingering and you want real answers, the next step is a proper evaluation. At Vivagen Health, our providers take the time to assess your full clinical picture before discussing whether testosterone therapy is right for you.
You do not need to diagnose yourself. You need a partner who can help you understand what is happening and what to do about it.Contact our experienced staff at our Coral Ridge Mall location at 954-440-6468 or our Broward Mall location at 954-372-2471 to schedule your testosterone therapy consultation today and get clearer answers about your symptoms.